Sleep Disorders: Symptoms, Diagnosis, and Treatment
- Key Takeaways
- What are Sleep Disorders?
- Obstructive Sleep Apnea (OSA)
- Narcolepsy
- Parasomnia
- Restless Legs Syndrome (RLS)
- Periodic Limb Movement Disorder (PLMD)
- Summary
- Glossary
Insomnia, or difficulty sleeping, is the most common sleep disorder and is discussed in detail in a separate article. This article will discuss other sleep disorders, including obstructive sleep apnea, narcolepsy, parasomnias, restless legs syndrome (RLS), and periodic limb movement disorder.
Key Takeaways
- There are many different types of sleep disorders. These disorders can affect a person’s quality of sleep, as well as their day-to-day functioning.
- Some sleep disorders may be managed with lifestyle changes or non-medication interventions, while others (like narcolepsy) may require treatment with medication.
What are Sleep Disorders?
Sleep is an essential bodily function, such as eating, drinking, and urinating. Sleep is not a luxury. When our body is deficient in sleep, parts of our system begin to malfunction. A sleep disorder exists when a bodily dysfunction affects your ability to fall asleep and stay asleep. There are over sixty diagnoses within seven categories of sleep disorder. Recognition is the first step toward addressing this critical medical issue. It is only then that treatment may be started.
Obstructive Sleep Apnea (OSA)
Obstructive sleep apnea (OSA) is a condition that causes apnea or interrupted breathing during sleep. It is the most common sleep disorder outside of insomnia, with approximately 15–30% of adult males and 5–15% of females in North America experiencing this condition. “Obstruction” refers to blockage or resistance to the airflow in your throat, leading to apnea.
Another type of sleep apnea (less common than OSA) is called central sleep apnea. In central sleep apnea, interrupted breathing occurs due to a problem in the brain. For example, central sleep apnea might happen after a stroke due to damage to the part of the brain involved in breathing.
On the other hand, OSA results from a physical problem: something in the upper airways blocking (obstructing) airflow. This blockage can be due to obesity, certain skull or facial abnormalities, vocal cord abnormalities, enlarged tonsils, swelling in the throat, or an enlarged tongue.
Because of the obstruction and related apnea, people with OSA do not get enough oxygen while sleeping. This can lead to some sleep apnea complications, such as heart problems.
Symptoms of Obstructive Sleep Apnea
Symptoms of OSA include:
- Daytime sleepiness.
- Snoring/choking/gasping while sleeping.
- Waking up with a headache.
- Waking up frequently during the night.
- Not feeling rested after a full night’s sleep.
- Having to urinate frequently at night.
The Epworth Sleepiness Scale can measure sleepiness. This scale measures how prone you are to falling asleep during everyday activities like reading, watching television, or driving.
Risk Factors for Obstructive Sleep Apnea
Risk factors for OSA include:
- Older age
- Being biologically male
- Obesity
- Structural problems in the upper airway
Structural problems that may cause OSA include enlarged tonsils/adenoids (especially in children) and jaw abnormalities that you are born with. Smoking and having a family history of OSA can also increase your risk of developing the condition.
Many medical conditions are associated with an increased risk for OSA. These include the following:
- High blood pressure (hypertension)
- Heart failure
- Strokes
- Abnormal heart rhythms, like atrial fibrillation
- Severe kidney disease
- Diabetes
- Pregnancy
- Acid reflux
- Parkinson’s disease
- Chronic lung diseases, such as COPD and asthma
- Low thyroid hormone levels (hypothyroidism)
- Polycystic ovary syndrome (PCOS)
Obstructive Sleep Apnea Diagnosis
If your doctor thinks you have sleep apnea, they will likely refer you to a sleep specialist and order a sleep study. Sleep studies use sensors on your head and body to monitor your oxygen levels, heart rate, breathing rate, snoring, body movements, and sleep stage while you sleep. These tests can be done in a sleep center or, in some cases, in your home.
Sleep apnea is important to identify and treat because it can lead to many serious complications, including:
- Car accidents related to drowsy driving.
- Cognitive problems, such as poor memory and concentration.
- Increased moodiness and depression.
- High blood pressure, heart attacks, heart failure, abnormal heart rhythms, and stroke.
- Diabetes.
- Fatty liver.
Although they can’t cure OSA, specific lifestyle changes can help reduce the severity of sleep apnea. These include:
- Weight loss.
- Avoiding alcohol and certain sedative medications like benzodiazepines, opioids, and some antihistamines.
- Getting enough exercise.
- Changing your sleeping position if this is an issue recognized during your sleep study.
Treatments for Obstructive Sleep Apnea
Prescription treatments are often needed to treat OSA. These include:
- Continuous positive airway pressure (CPAP). This device administers a small amount of pressure through your nose and mouth to keep your upper airway open while you sleep. It can take some getting used to, and sometimes adjustments must be made. However, a CPAP machine can make a difference in reducing apnea and improving your sleep quality.
- Oral appliances. These are usually recommended if CPAP has not worked for you and you have mild-to-moderate sleep apnea. The appliance is usually a splint or other device you wear in your mouth at night that helps to keep your airway open.
- Upper airway surgery. This is typically only recommended when some physical issues, such as enlarged tonsils or jaw abnormalities, cause OSA.
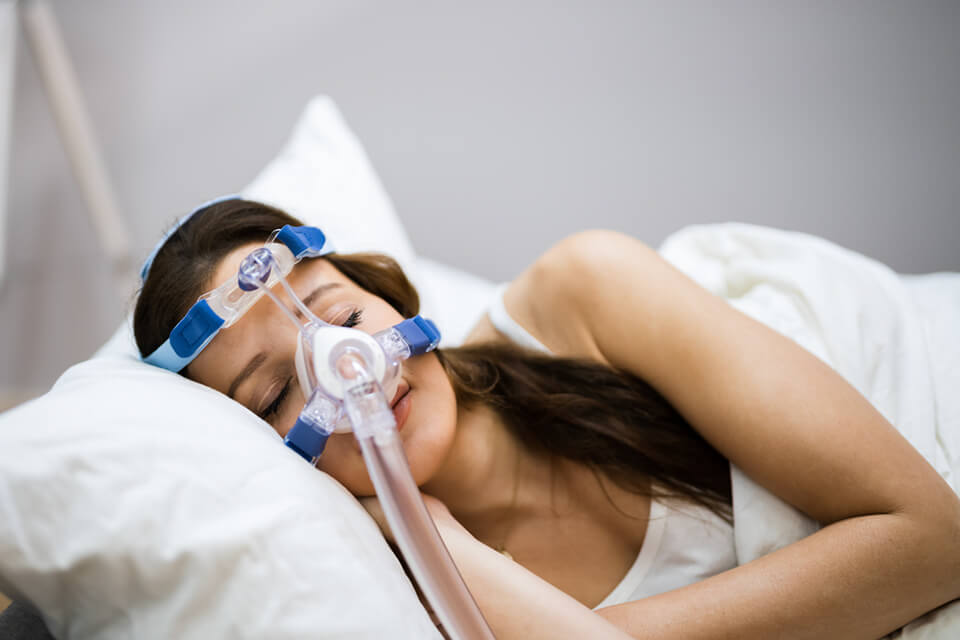
Example of a continuous positive airway pressure (CPAP) device.
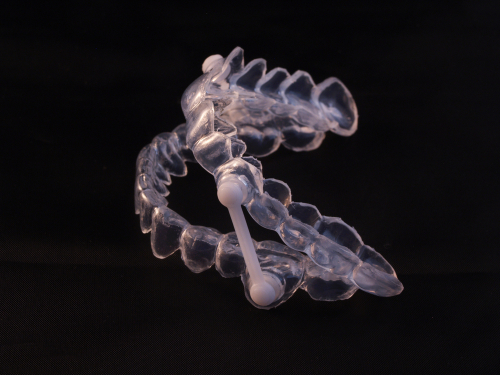
Example of oral appliance used for treatment of obstructive sleep apnea.
Narcolepsy
Narcolepsy is a rare sleep disorder that affects fewer than 1 in 10,000. It is a disorder that affects the control of your sleep-wake cycle. This means that some elements of sleep occur during the day, and some elements of being awake occur when you sleep.
Just like with OSA, if you have narcolepsy, you will likely experience daytime sleepiness. However, you will likely also have additional symptoms, such as cataplexy (sudden loss of muscle control), hallucinations as you fall asleep, and Sleep paralysis (awake but unable to move).
Although narcolepsy can run in families, it sometimes does not, and the cause is often unknown. It is known that in some types of narcolepsy, there is a deficiency in a specific neurotransmitter called orexin. Orexin is made in the brain and is involved in keeping you awake. However, the cause of low orexin levels in people with narcolepsy is not yet known. In some rare cases, people with narcolepsy have a problem in the part of the brain that makes orexin, such as a tumor, stroke, or another process that causes an injury affecting orexin levels.
Symptoms of Narcolepsy
Symptoms of narcolepsy include excessive daytime sleepiness, cataplexy, hallucinations, and sleep paralysis.
Daytime Sleepiness
As with OSA, daytime sleepiness is a symptom experienced by most people with narcolepsy. This sleepiness can be evaluated with the Epworth Sleepiness Scale. In narcolepsy, daytime sleepiness is moderate to severe. If you have narcolepsy, you might doze off with a minimal warning in a “sleep attack.” Unlike OSA, after a brief nap, you feel rested again.
Cataplexy
This is an unusual experience where a strong emotional reaction, such as laughter or excitement, triggers muscle weakness. Negative emotions, such as fear or anger, can also cause cataplexy, but they aren’t as commonly a trigger. Cataplexy almost always starts in the face with drooping eyelids and an open mouth but can progress to collapse due to total body weakness. You remain awake during cataplexy, and it goes away in a minute or two.
Hallucinations
People with narcolepsy may experience hallucinations just before falling asleep (hypnagogic hallucinations). You may see, hear, or even feel something that isn’t there. This can be quite vivid and frightening. Less commonly, these hallucinations can occur right after waking up (hypnopompic hallucinations).
Sleep paralysis
Sleep paralysis usually occurs in narcolepsy for one to two minutes immediately after you wake up, but it can also occur just before falling asleep. During sleep paralysis, you feel awake but cannot move. Sometimes, this can feel frightening and be accompanied by a hallucination of feeling suffocated. Sleep paralysis and hallucinations related to falling asleep can occur rarely (once every few years) and be normal. With narcolepsy, they happen much more frequently.
Narcolepsy Diagnosis
Your doctor will determine if you have narcolepsy based on your symptoms and the results of some specialized sleep tests. The sleep testing is similar to what is outlined above for OSA, with the addition of a multiple sleep latency test (MSLT). This exam measures how long it takes for you to fall asleep for a nap during the daytime. A person with narcolepsy will fall asleep and enter rapid eye movement (REM) sleep faster than usual.
While your family doctor, pediatrician, or internal medicine doctor might start your evaluation for narcolepsy, most people will be diagnosed and followed by a sleep specialist. It is not uncommon for people with narcolepsy to have other sleep disorders.
One of the main complications of narcolepsy is car accidents caused by excessive sleepiness. Long drives on the highway are often the most difficult. You should talk to your doctor about driving safety with narcolepsy.
Narcolepsy Treatments
There are both lifestyle and medication treatments for narcolepsy. Lifestyle treatments include the following:
- Naps. Even for just 20 minutes, taking a nap or two can help improve daytime sleepiness.
- Good, consistent sleep. It is important to keep your sleep schedule regular and get enough quality sleep.
- Avoiding certain medications or substances. Any substance that is sedative or makes you drowsy can worsen daytime sleepiness. This can include opiates, benzodiazepines, and alcohol. On the other hand, substances that cause insomnia, including caffeine, can also worsen daytime sleepiness.
- Psychological support. Depending on the severity of your narcolepsy, you might have significant challenges functioning at work and home. Additionally, many people do not understand symptoms like sleep attacks and cataplexy. Sometimes, they can be misunderstood as being purposeful actions. There is also an increased risk for anxiety and depression with narcolepsy. For all these reasons, you may be helped by counseling or a narcolepsy support group.
- Diet and exercise. While a healthy diet and exercise are always helpful for general health, they are vital for people living with narcolepsy. Weight problems are common. This may be due to metabolism changes, but the cause isn’t apparent. Regular exercise and appropriate diet are important to minimize weight gain.
Your doctor may recommend or prescribe medications that can be helpful for excessive daytime sleepiness, as well as medications to reduce episodes of cataplexy. These drugs are typically stimulants or work by affecting neurotransmitter levels. The proper medications for you will depend on your symptoms and your overall health.
Many people do not understand symptoms like sleep attacks and cataplexy. Sometimes, they can be misunderstood as being purposeful actions. There is also an increased risk for anxiety and depression with narcolepsy.
Parasomnia
Parasomnia is a general term for unusual behaviors that people experience related to sleep. In the past, many of these were thought to be psychological in nature. However, most are now known to be medical disorders of sleep or the different stages of sleep.
Several common parasomnias are listed below. In most cases, treatment is unnecessary for confusional arousals, sleep terrors, or sleepwalking. Maintaining a regular sleep schedule and getting adequate sleep decreases all parasomnias.
Sleep Terrors
Sleep terrors (also known as night terrors) are episodes resembling nightmares. Sleep terror is a type of parasomnia. Unlike nightmares, these episodes are very violent or dramatic, often causing a person to scream, thrash or kick, sweat, or breathe rapidly.
A person experiencing sleep terrors may partially awaken or bolt upright in bed. They will appear awake to others but not respond to those around them. You may also remember having the sleep terror but not recall any details.
Sleep terrors occur between two and three hours into sleep during the transition from deep non-REM sleep to light REM sleep. These episodes only last a few minutes before a person falls back asleep.
Sleep terrors often run in families and are more common in children. Sometimes, other sleep disorders trigger sleep terrors.
Confusional Arousals
Confusional arousal is a parasomnia that refers to feeling disoriented or confused after waking up. This may last up to 10 minutes. Afterward, you won’t remember what you did during this time. These episodes are more common in children. They are not dangerous, and it is best to wait for the episode to resolve rather than interrupt a person while it is happening.
Sleepwalking
Sleepwalking refers to moving about or performing complex tasks while mostly asleep. It occurs during deep non-REM sleep (stage III of the sleep cycle). Like some other parasomnias, sleepwalking is more common in children than adults.
People who sleepwalk will not respond fully to their surroundings, and can be hard to wake up. Because they tend to be clumsy, they can easily injure themselves by tripping or falling. Episodes of sleepwalking tend to occur early at night and last for 15 minutes or less. Usually, the sleepwalker then goes back to bed and continues to sleep. Sleepwalkers can become agitated, aggressive or even violent if you try to wake them up.
If a sleepwalker has had an injury, ensuring their safety is essential. You will need to look at what can be done to keep that person safe. This may include securing sharp objects, blocking access to stairs and windows, padding furniture or the floor, and locking doors. Suppose sleepwalking is particularly problematic (dangerous or otherwise undesirable consequences have occurred). In that case, your doctor may recommend evaluating you for other sleep disorders, stopping medications that affect sleep, or switching you to more effective sleep medications.
To keep sleepwalkers safe, you may need to secure sharp objects, block access to stairs and windows, pad furniture and lock doors.
Sleep-Related Eating Disorder (SRED)
Sleep-related eating disorder (SRED) involves sleepwalking and then eating in a binge fashion. Most people recall being “half asleep” during these episodes. This parasomnia can lead to serious health consequences, including obesity, high cholesterol, diabetes, cavities, or injuries from burns or utensils.
Women are more commonly affected by SRED than men. Treatment for SRED includes the evaluation and treatment of any other sleep disorder. It may also involve specific medication options.
REM-Sleep Behavior Disorder (RBD)
REM-sleep behavior disorder affects the period of sleep known as rapid eye movement (REM) sleep. In this condition, people act out their dreams. For instance, a person may punch, kick, talk, swear, or jump out of bed. People usually remember having violent or threatening dreams. This disorder can be dangerous to the individual or your bed partner.
RBD is more common in individuals 50 and older. It is also more common in men than in women. RBD may occur during withdrawal from alcohol or sedatives, such as benzodiazepines and barbiturates, and can develop as a side effect of certain psychiatric medications. RBD is also associated with Parkinson’s disease and Lewy body dementia– both degenerative neurological disorders.
As with sleepwalking, safety is important for those with RBD. Your doctor will look at any psychiatric medications you take to ensure they are not related to your symptoms. Several prescription medications are available for treating RBD. Melatonin (sometimes in prescription doses) is also a treatment option. Your doctor will work with you to decide which medication is best for you based on your symptoms, the safety of each medication based on your underlying health, and any potential side effects.
Nightmares
Everyone has bad dreams from time to time. Nightmares are not usually associated with movements (such as sitting up or lashing out, as seen with sleep terrors). Often, a person will remember their nightmare and may feel anxious or fearful when they wake up.
Stressful events may be triggers for nightmares. Certain medications, as well as withdrawal from certain medications, can also trigger nightmares. Although nightmares are more common in children, they still occur commonly at any age.
Like other parasomnias, nightmares may be managed by normalizing sleep with a regular sleep schedule and adequate sleep and minimizing medication triggers. If nightmares are causing significant stress in your life, they should be addressed. Your doctor might refer you to a counselor for additional help. Your doctor may also consider certain medications if your nightmares are severe, persistent, or not responding to non-medication treatments.
Restless Legs Syndrome (RLS)
Restless legs syndrome (RLS) is a common sleep disorder that causes an uncomfortable urge to move your legs in the evening or while trying to sleep. If you get up and move, you feel better, but only for a short time. Sometimes, you may also experience these feelings during the day.
Some people have difficulty describing what RLS feels like. They may call it “creeping,” “pulling, “crawling,” “tingling,” or “cramping” sensations, for example. The cause of RLS is unknown, although research focuses on nervous system problems.
Causes and Risk Factors of Restless Legs Syndrome
There are many risk factors for RLS. The most common are listed below.
- Family history. About 50% of people with RLS have someone in their family with it.
- Low iron levels. Even without anemia, low iron levels are strongly associated with RLS. Research has shown that low iron levels in the brain can be associated with RLS, even in people with normal blood iron levels.
- Kidney failure. People with kidney disease may develop RLS if they do not receive adequate blood dialysis.
- Spinal cord disease. Injury, tumors, infections, and degenerative spinal cord conditions are all associated with RLS. Spinal cord blocks for anesthesia can also cause or worsen RLS.
- Pregnancy. About 25% of women develop RLS during their pregnancies. Symptoms tend to worsen over time and go away shortly after delivery.
- Multiple sclerosis (MS). Studies show that 10–60% of people with MS also have RLS.
RLS symptoms worsen with time and can lead to poor sleep, depression, and anxiety. Rarely, the arms may also be involved (usually only in severe, long-lasting cases). However, a significant number of people with RLS experience spontaneous remission, which means the symptoms go away on their own without apparent reason. Most people with RLS also have PLMS (periodic limb movements of sleep), which is discussed later in this article.
Certain medications can make RLS worse. You should discuss your medications with your doctor if you have RLS.
- Antihistamines. Particularly the older antihistamines that make you drowsy, like diphenhydramine and chlorpheniramine. These are available over the counter and are used for allergies, colds, and sleep symptoms.
- Dopamine receptor agonists. This is a class of medications, including prescription anti-nausea medications that are also used in migraine disorders, including prochlorperazine, chlorpromazine, and metoclopramide, as well as some antipsychotic medications.
- Antidepressants.
Restless Legs Syndrome Diagnosis
There is no specific test for RLS. Your doctor will provide a diagnosis based on your symptoms. However, everyone with RLS symptoms should have a lab test performed to assess their iron levels (and possibly kidney function if kidney failure is suspected). Sleep studies are only done if the diagnosis is unclear or other sleep disorders are suspected. Sometimes a nerve conduction study and an electromyogram are done if your doctor wants to rule out neuropathy.
Restless Legs Syndrome Treatment
As with other parasomnias, lifestyle changes and medication options are available for managing RLS. However, the first treatment to consider for everyone with RLS is iron replacement. Experts recommend iron supplementation if a person’s fasting ferritin level is 75mcg/L or less. This level should be continuously monitored to be sure it is enough but not too much, as there can be side effects from too much iron (iron overload).
Non-medication interventions may be adequate in mild cases of RLS. However, they are also important in more severe cases, as they can help to limit the amount of medication needed. Some of these lifestyle changes are listed below.
- Keep your mind active. Avoiding times of rest or boredom, particularly in the evening, can decrease RLS symptoms. Working on a crossword puzzle, reading, or journaling are some examples.
- Avoid aggravating substances or factors, such as certain medications and caffeine.
- Get moderate regular exercise.
- Try symptom relief techniques when your legs are bothering you, such as walking or other physical movements, soaking, and massage.
- Practice good sleep hygiene. The importance of a regular sleep schedule and adequate sleep cannot be overstated. Talk to your doctor if you are having problems getting enough quality sleep.
- Evaluate and treat other sleep disorders. Your doctor will help you with this. It is common to have more than one sleep disorder, and you will not receive the fullest possible symptom relief if there is another unknown sleep disorder.
- Alternative therapies. Yoga and acupuncture may have some benefits, but other herbal and complementary therapies need more scientific studies to determine their usefulness.
If your RLS is not responding to these therapies and is affecting your well-being and functioning, your doctor may consider medication treatment for your RLS. Some people only need medications when they have a bad day or night, while others need to take medication daily for their RLS.
As with most conditions, the decision on which medication to take is made between you and your doctor based on your symptoms, the safety of the medications given your underlying health, and any potential side effects.
The first treatment to consider for everyone with RLS is iron replacement. Experts recommend iron supplementation if a person’s fasting ferritin level is 75mcg/L or less. This level should be continuously monitored to be sure it is enough but not too much, as there can be side effects from too much iron (iron overload).
Periodic Limb Movement Disorder (PLMD)
A “periodic limb movement” is when you repeatedly move part of your arm or leg during your sleep, always the same way. For example, you might slightly flex your big toe multiple times in a row, or another person might bend their whole leg (or both legs) three times in a row. Regardless of the movement, it is the same movement every time.
It is normal to experience some of these limb movements while sleeping, which is increasingly common with age. You may be completely unaware until your bed partner tells you about them. Periodic limb movement disorder (PLMD), on the other hand, is uncommon. People with PLMD experience more than 15 periodic limb movements per hour and other negative effects on their sleep.
Most people with PLMD do not have insomnia but may wake up from their movements. Daytime sleepiness is usually the main complaint that leads people to see their doctor. Your doctor will use your symptoms, health history, and a sleep study to diagnose you with PLMD. Treatment for PLMD is similar to RLS. However, the data on PLMD, including treatment, is more limited than on other sleep disorders.
Risk Factors of Periodic Limb Movement Disorder
PLMD shares some of the same risk factors as RLS, such as kidney failure and spinal cord disease, but they are considered separate disorders. If you have RLS, you will likely have periodic limb movements while you sleep. PLMD is associated with multiple other sleep disorders. Some medications that worsen RLS (like some antidepressants) can also worsen PLMD. Sometimes, the overlap in these two disorders can make diagnosis more difficult.
Summary
There are over sixty diagnoses involving sleep disorders. Just as the diagnosis are varied, so are the cause and treatments. Recognition of the sleep disorder(s) that affects you is essential to your treatment and overall health. Proper sleep is not simply a luxury but an essential bodily function. Doing all you can to maintain proper sleep hygiene will go a long way in mitigating or preventing certain chronic conditions and improving your quality of life. It is well worth the effort.
Glossary
- Antipsychotic medications treat severe mental disorders, such as those that cause a loss of touch with reality. These medications may also treat depression and anxiety ( usually in lower dosages).
- Apnea is the stopping and starting of breathing during sleep.
- Cataplexy is a collapse due to a sudden loss of muscle control, often triggered by strong emotions such as laughter, fear, anger, or excitement.
- Electromyogram is a test often done with a nerve conduction study to further assess nerve health. For this test, a small needle is placed in the muscle that the nerve goes to, and electrical measurements are taken from the needle.
- Ferritin test is a blood test done to check iron levels. Ferritin is a protein that stores iron in the body.
- A nerve conduction study is a test used to detect nerve damage by measuring how electrical impulses move through the nerve. For this test, a small shock is given to the nerve in your arm or leg where the nerve is located. While you can feel this, it isn’t usually considered painful.
- Neuropathy is an abnormality with a nerve or nerves in the arms or legs.
- Neurotransmitters are chemicals that nerves use to communicate with each other and other body parts.
- Sleep paralysis is a feeling of being awake but unable to move.
- Upper airways refer to the parts of the body above the lungs and trachea (windpipe) that air flows through. The upper airways include the nose, mouth, and throat.
Copyright: myObMD Media, LLC | Written by: myObMD Physician Author | Edited by: Victoria Menard and Dayna Smith, MD | January 16th, 2023.
References
- Judd, B. G., & Sateia, M. J. Classification of sleep disorders. UpToDate. Retrieved from https://www.uptodate.com/contents/classification-of-sleep-disorders.
- Badr, M. S. Pathophysiology of upper airway obstruction in obstructive sleep apnea in adults. UpToDate. Retrieved from https://www.uptodate.com/contents/pathophysiology-of-upper-airway-obstruction-in-obstructive-sleep-apnea-in-adults.
- Hensley, M., & Ray, C. (2010). Sleep apnea. American Family Physician, 81(2), 195. PMID: 20082516
- Kline, L. R. (2022, November 17). Clinical presentation and diagnosis of obstructive sleep apnea in adults. UpToDate. Retrieved from https://www.uptodate.com/contents/clinical-presentation-and-diagnosis-of-obstructive-sleep-apnea-in-adults.
- Kryger, M. H., & Malhotra, A. (2022, August 11). Management of obstructive sleep apnea in adults. UpToDate. Retrieved from https://www.uptodate.com/contents/management-of-obstructive-sleep-apnea-in-adults.
- Scammell, T. E. Clinical features and diagnosis of narcolepsy in adults. UpToDate. Retrieved from https://www.uptodate.com/contents/clinical-features-and-diagnosis-of-narcolepsy-in-adults.
- Scammell, T. E. Treatment of narcolepsy in adults. UpToDate. Retrieved from https://www.uptodate.com/contents/treatment-of-narcolepsy-in-adults.
- Markov, D., Jaffe, F., & Doghramji, K. (2006). Update on parasomnias: a review for psychiatric practice. Psychiatry (Edgmont), 3(7), 69–76. PMID: 20975819; PMCID: PMC2958868.
- Ondo, W. G. Clinical features and diagnosis of restless legs syndrome and periodic limb movement disorder in adults. UpToDate. Retrieved from https://www.uptodate.com/contents/clinical-features-and-diagnosis-of-restless-legs-syndrome-and-periodic-limb-movement-disorder-in-adults.
- Silber, M. H. (2022, June 29). Management of restless legs syndrome and periodic limb movement disorder in adults. UpToDate. Retrieved from https://www.uptodate.com/contents/management-of-restless-legs-syndrome-and-periodic-limb-movement-disorder-in-adults.
Suni, E. (2022, October 7). Sleepwalking: What is Somnambulism? Sleep Foundation. Retrieved from https://www.sleepfoundation.org/parasomnias/sleepwalking.


