Fibromyalgia Your Complete Guide
- What is fibromyalgia?
- Fibromyalgia Symptoms
- What causes fibromyalgia?
- What Makes Fibromyalgia So Difficult to Treat-Central Sensitization
- How do I know if I have fibromyalgia?
- What is the difference between a tender point and a trigger point?
- What other disorders can look like fibromyalgia?
- Is fibromyalgia a real disease, or is it “all in my head”?
- What has fibromyalgia research discovered?
- Is fibromyalgia an autoimmune disease?
- Is there a cure for fibromyalgia?
- How is fibromyalgia treated?
- What are lifestyle and natural treatments for fibromyalgia?
- What are the best medications for fibromyalgia?
- Can I take opioids for fibromyalgia?
- What if my treatment is not working?
- Fibro and Other Chronic Pain Conditions
- What are some alternative treatments for fibromyalgia?
- What is fibromyalgia?
What is fibromyalgia?
Fibromyalgia (“fibro”) is a long-lasting condition that causes pain all over the body. In the US, 2-8% (10 million) people are affected with fibromyalgia. Each person’s symptoms may vary, and the pain can shift throughout your body.
Fibromyalgia causes your muscles and the places where your muscles attach to bone (tendons and ligaments) to become unusually tender or sensitive to touch. Other common symptoms include trouble sleeping, fatigue, anxiety, and depression. We do not know what causes fibromyalgia. It may be due to a change in how your brain and nerves process pain.
While it can significantly affect a person’s quality of life, fibro does not shorten your life. There is no cure, but there are treatments that can help you.
Fibromyalgia Symptoms
- Pain and stiffness in muscles and joints all over your body.
- Difficulty Sleeping.
- Headaches, including migraines, are present in about 50% of fibro sufferers.
- Depression or anxiety affects up to half of the people diagnosed with fibromyalgia.
- Poor memory and concentration.
- Abnormal skin sensations. Numbness, tingling, burning, or “creepy-crawly” sensations, often in the arms and legs.
- Pain in the jaw or face.
- Gastrointestinal problems such as pain, bloating, constipation, or irritable bowel syndrome.
Fibromyalgia may also cause pain in your chest muscles, chronic pelvic pain, dry eyes, cold sensitivity in your fingertips (Raynaud’s Syndrome), acid reflux, hearing loss, and frequent urination.
What causes fibromyalgia?
The cause of fibromyalgia is unknown. We know that being female, middle-aged, and having certain conditions increase your risk of developing fibromyalgia.
Conditions That Increase Fibromyalgia Risk
- Age- middle age is the most common time for fibromyalgia to develop, although it can affect people at any age, including during childhood.
- Lupus or rheumatoid arthritis are two autoimmune disorders that commonly affect your joints and increase your risk of fibromyalgia.
- Female Gender- women get fibro twice as often as men.
- Repetitive joint injuries.
- Family history of fibromyalgia.
- Viral or other illnesses.
- Stressful or traumatic events such as car accidents, childhood traumas, PTSD.
What Makes Fibromyalgia So Difficult to Treat-Central Sensitization
Medical experts believe hypersensitivity and pain processing issues cause fibromyalgia in the central nervous system and brain. This hypersensitive pain processing is called central sensitization. Your brain remains highly alert and may perceive normal sensations as painful and mildly painful sensations as severe. Generally, if you strain your shoulder, the pain you feel comes directly from the shoulder. It is different if you have fibromyalgia.
In fibromyalgia, your brain is on high alert and may perceive normal sensations as painful and mildly painful sensations as severe.
If your shoulders are hurting from fibromyalgia, it is not because they are injured. The sensation of shoulder pain is due to a problem with the nerves in your brain and central nervous system. That explains why the usual treatments used for shoulder pain, such as ibuprofen and heat, do not work as well for fibromyalgia pain. Traditional pain medicines do not target the source of the pain.

How do I know if I have fibromyalgia?
There is no specific blood test or x-ray available for diagnosing fibromyalgia. Fibromyalgia is a clinical diagnosis. A clinical diagnosis means your doctor diagnoses the problem based on your history and physical exam findings, not a blood test or imaging. However, your doctor may decide to do lab tests or imaging studies to help rule out other conditions.
There are two blood tests called ESR and a C-reactive protein (CRP). These are called inflammatory markers, and they look for evidence of inflammation in your body. The ESR and CRP tests are usually normal with fibromyalgia. If these test results are high, it suggests that you DO NOT have fibromyalgia. Your doctor will investigate for a different diagnosis. Your doctors may also do blood tests to rule out thyroid disease.
If you have fibromyalgia, your physical exam will likely be normal. There are usually no visible swellings, discolorations, areas of numbness, or muscle weakness. There is, however, increased tenderness in soft tissue areas called tender points.
What is the difference between a tender point and a trigger point?
A tender point refers to areas in the soft tissue that are abnormally sensitive or tender to touch or pressure. Tender points are specific to fibromyalgia, are on both sides of your body, above and below your waist. In the past, doctors used eighteen specific tender points to diagnose fibro. Now, many doctors feel those specific points are not necessary.
If you have at least three months of widespread soft tissue tender points, even if they are not in the classic locations for fibromyalgia, you can be diagnosed with fibro.
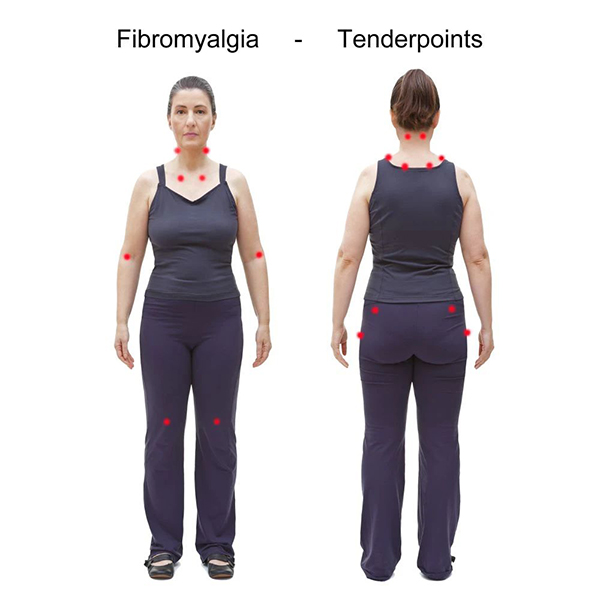
Classic Tender Point Locations:
- Where your head meets your neck in the back.
- Trapezius muscle is at your upper back between the neck and shoulder.
- Upper shoulder blade.
- The upper outer portion of your buttocks.
- Just behind the point of your hip on the side of your upper leg.
- The lower part of your neck, in front.
- The junction between the upper part of your breastbone and your rib.
- Outer elbow
- Inner knee
Trigger points, on the other hand, are not seen in fibromyalgia. Trigger Points are associated with myofascial pain syndrome. A trigger point is usually located in a tight band of muscle and is a specific spot that, when pressed, is very irritable. Pressing on a trigger point may make your muscle cramp and cause pain in distant sites. Pain originating in one area but felt in another area of your body is called referred pain.
Tender points and trigger points can be easily confused, which is why the diagnosis of fibromyalgia no longer involves the use of tender points. Myofascial pain syndrome and fibromyalgia have a lot of overlapping symptoms. They both involve central sensitization and may develop from common genetic and environmental triggers like stress and sleep problems.
Although fibromyalgia and myofascial pain syndrome resemble each other, they are different conditions. Fibromyalgia and myofascial pain syndrome are distinguished based on physical history and examination findings. The most significant difference between the two is that fibromyalgia occurs all over the body, while myofascial pain concentrates in one specific area (trigger point).
What other disorders can look like fibromyalgia?
Myofascial Pain Syndrome Myofascial Pain Syndrome causes pain that concentrates in one body area. This area is called a trigger point. Fibromyalgia pain is random and all over the body. The pain sites in fibromyalgia are tender points. The pain site for myofascial pain syndrome is a trigger point.
Neuropathy is a disorder of nerves or muscles that can cause numbness or muscle weakness. Fibromyalgia does not cause weakened and numb muscles.
Inflammatory arthritis is a disorder with joint inflammation due to an overactive immune system, as in rheumatoid arthritis and lupus arthritis. Often ESR and CRP blood tests are elevated. These things differentiate it from fibromyalgia.
Lyme disease is transmitted to humans by deer ticks. Typical symptoms include fever, headache, fatigue, and a characteristic skin rash. If left untreated, the infection can spread to joints, the heart, and the nervous system. It’s essential to contact your doctor if you have joint swelling or a “bulls-eye” rash. Your doctor might decide to test you for Lyme disease.
Polymyalgia rheumatic (PMR) is a disorder that occurs in persons over 50 years old and is associated with inflammation in the muscles and joints. Unlike fibromyalgia, in PMR, lab tests show high inflammatory markers like ESR and CRP.
- Myositis is an uncommon family of inflammatory muscle disorders. If you have muscle weakness and tenderness, your doctor may want to test you for myositis.
Is fibromyalgia a real disease, or is it “all in my head”?
Fibromyalgia is a well-established medical condition. It is very much a real disease. Unfortunately, if you have fibromyalgia, you may experience the stigma of doubt because this is considered an “invisible disease.” Others cannot see what you feel. There is no rash, no joint swelling, or a definitive lab test. Some people believe that you are faking your symptoms or that your symptoms stem from emotional problems. This stigma makes life even harder for people with fibro.
Having no physical manifestations may cause others to doubt your fibromyalgia symptoms.
What has fibromyalgia research discovered?
Even though there is no specific test for fibro, scientific research and specialized brain scans of those living with fibromyalgia show specific changes in the brain.
People with fibromyalgia have abnormal levels of certain neurotransmitters in the areas of their brain responsible for processing pain.
- Communicative areas of the brain lack normal connectivity. Some parts of the brain are hypersensitive to pain.
- Grey matter decreases with fibromyalgia, chronic pain disorders, and premature aging.
Although fibro research may not impact your current everyday life, it does help us better understand the disease and eventually leads to new and more effective treatments. Research findings remind us that fibro is a real disorder that is not yet fully understood.
Is fibromyalgia an auto-immune disease?
Currently, there is no evidence that fibromyalgia is an auto-immune condition. Fibro is likely a neurological disease. While the cause of fibromyalgia is unknown, the best evidence points to this being a neurological disease affecting nerve and brain function. There continues to be ongoing research to determine a possible link to autoimmune disease.
Is there a cure for fibromyalgia?
Although there is currently no cure for fibromyalgia, multiple treatment options are available. Having fibromyalgia does not increase your risk of death, nor does it cause damage to other organs in your body. It tends to be a lifelong, non-progressive, chronic disease with symptoms that come and go.
How is fibromyalgia treated?
Fibromyalgia is treated by primary care physicians (PCPs), internists, and even pediatricians. A doctor who specializes in treating fibromyalgia is called a rheumatologist.
While there are many different treatments for fibromyalgia, a combination of varying treatment options works best. Treatments are either medications or lifestyle changes.
What are lifestyle and natural treatments for fibromyalgia?
When you are ill, especially with a chronic condition like fibromyalgia, for the best results, medication should NOT be your only approach to treatment.
It is best to consider multiple treatment modalities.
Exercise. Physical activity is an essential aspect of staying healthy. It is also important if you have fibromyalgia. In addition to all the known health benefits, exercise helps to counteract the central sensitization found in fibromyalgia. Studies show that people with fibromyalgia who are active do better in the long run than sedentary people.
Many people with fibromyalgia find exercise painful and fatiguing. Finding the right amount of exercise that benefits you without causing your fibromyalgia to flare can take time. Your physician can help by referring you to a physical therapist who can assist you in developing the right exercise program for you.
You can do 30 minutes, five days a week, or break it up into intervals that work best for you. Even if 150 minutes weekly is too much for you, studies show that doing any physical activity is better than doing none. Most people find that they can increase their intensity and duration of exercise over time.
Taking a class at a local community center can be an excellent way to start exercising. Be sure to start slow with gradual increases as you go along. Folks with medical problems affecting their exercise ability, men over age 40 and women over age 50, should consult their doctor before beginning a new exercise program.
Your breathing pattern while exercising can indicate the intensity of your workout. A light effort will allow you to carry on a conversation with ease while exercising. A moderate effort workout will allow you to speak, but long conversations will be difficult. If you have trouble speaking even a few sentences, your exercise level is vigorous.
Stress management. One of the most commonly recommended stress management techniques involves mindfulness. Mindfulness is a technique where you focus your awareness on the present moment and, over time, train your mind to be calmer. Being mindful is a skill that develops with time. The more often you practice, the better you will become.
- Healthy sleep habits.Fibromyalgia can cause sleeping difficulty. Other conditions such as restless legs syndrome (RLS), obstructive sleep apnea (OSA), or insomnia can also make restful sleep difficult. Consult your physician if you aren’t sleeping well to determine the actual cause.
Healthy Sleep Habits
- As much as possible, go to bed and get up at the same time each day, including weekends.
- Avoid regular daytime naps.
- Develop a night-time routine that is calming and gets your brain ready for sleep: journal, read, listen to quiet music, take a relaxing bath, meditate.
- Make sure your room is dark, quiet, and at a comfortable temperature for sleep.
- Exercise regularly, but avoid exercise within 4 hours of sleep.
- Avoid alcohol near bedtime.
- Avoid smoking, particularly in the evening.
- Avoid caffeine after 2 pm.
- Avoid large meals and limit fluids right before bed.
- Do not go to bed hungry.
- Minimize screen time before bed. Turn off your phone, computer, and television.
- Address any stressors or worries before you go to bed. Journaling can be helpful—practice gratitude.
- If you cannot fall asleep after 20 minutes, get out of bed and do a quiet activity until you feel sleepy again, then go back to bed. Do not read, sew, watch television, etc., in bed. The bed should be for sleeping and intimacy only.
Cognitive Behavior Therapy (CBT) or “talk therapy.” With CBT, your therapist will help you identify helpful thinking or action patterns and those that aren’t. The goal is to make changes in those patterns in learning better ways of coping.
While CBT is great, it may not work for everyone. There are many different types of therapy, and your counselor can adjust to your specific needs. Talk therapy may be of particular benefit to you if you have an underlying mood disorder such as anxiety or depression. For those suffering from chronic pain, talk therapy helps to learn how to better cope with your illness.
Group Educational Classes. Your doctor may be able to refer you to a class in your area designed to help people with chronic conditions better understand their illness. This knowledge can give you confidence in controlling your symptoms and living better with fibro.
What are the best medications for fibromyalgia?
There are a lot of factors that go into deciding the best medication for you. Your predominant fibromyalgia symptoms, your medical and medication history, drug interactions, and side effects are all aspects your provider must consider. Therefore, only you and your doctor can decide the best medication to take for fibromyalgia. However, this section will give you some ideas to discuss with your doctor.
- Tricyclic antidepressants (TCAs). TCAs include amitriptyline, desipramine, and a related muscle relaxant called cyclobenzaprine. These are usually given in a low dose at night and can help with pain, fatigue, and sleep. Tricyclic antidepressants are helpful in many painful conditions that have an underlying neurological cause, such as diabetic neuropathy, migraine, and irritable bowel syndrome. Even though these medications treat depression, they are also helpful in fibro and other chronic pain conditions.
We do not yet know precisely how TCAs work to relieve fibro symptoms. Likely, TCAs change the level of chemicals in your brain called neurotransmitters. Neurotransmitters are chemicals your nerves use to communicate with each other. The TCA dosages used in fibro are generally lower than the dosage used for depression. Some of the common side effects these medications can cause include dry mouth, drowsiness, and constipation. Older persons are more prone to side effects, including severe side effects like low blood pressure. TCA is a class of medication with one of the lowest costs. It is often tried first for fibro.
TCAs can cause nausea, dry mouth, constipation, drowsiness, headache, dizziness, and insomnia. Serious side effects are rare. These medications may be started at a low dose and increased to a full dose over time.
- Selective Norepinephrine Uptake Inhibitors (SNRIs). SNRI is another class of medications that we don’t know precisely how they work in fibro. Like TCA, SNRI works by changing neurotransmitter levels, although in different ways. Examples of SNRIs include duloxetine and milnacipran. Venlafaxine is an SNRI, but the data on venlafaxine on fibro is limited.
- Seizure medications.Pregabalin and gabapentin are both medications used for preventing seizures and can also help treat fibro. Both of these medicines help with sleep and might be a good choice if poor sleep is a particular problem for you. Effective dosing for these medicines vary. You may find a low dose beneficial, while others require a high dose to see a benefit. Common side effects include dry mouth, drowsiness, dizziness, swelling, and weight gain.
- Other medications, such as memantine, pramipexole, quetiapine, and other antidepressants, are used in fibromyalgia. They may not be as beneficial as those listed above but are things your doctor might consider if you do not respond to the more traditional medications.
While serious side effects are rare, all these medications can cause depression symptoms or even suicidal feelings. Tell your doctor immediately if this happens to you. Call 911 at 1-800-273-TALK (8255) if you are suicidal or in crisis.
It can take a while for these medications to kick in and start to work. So, your doctor may want you to take them for a few months before switching to something else, often gradually increasing the dose over that time, as long as you do not have side effects.
Many people with fibromyalgia have had it a long time before being diagnosed. You may have already tried over-the-counter medications for your chronic pain with little or no benefit. While the over-the-counter drug may not work on long-lasting pain, it may still help relieve short-lived fibromyalgia flare.
Over-the-counter drugs such as aspirin, ibuprofen, naproxen, and acetaminophen are for sporadic use. Long-term use of these drugs can cause side effects like liver, kidney, heart problems, stomach and intestinal ulcers, heart attacks, and strokes. If you find yourself reaching for these medicines frequently, talk to your doctor about whether they are safe for you to take.
Can I take opioids for fibromyalgia?
If you and your doctor are considering using opioids for treating your fibromyalgia, there are some things you need to consider. Opioids are also called narcotic medications and include things like codeine, hydrocodone, hydromorphone, morphine, and fentanyl. While it might seem to make sense to take a painkiller like this for a painful condition like fibromyalgia, research has shown that opioids are not helpful in fibro and do more harm than good.
Opioid side effects include depression, drowsiness, addiction, increased sensitivity to pain, heart and breathing problems, constipation, and hormonal problems, including sexual dysfunction. People with fibro who take opioids do poorer overall than people who do not take this class of medications. Talk to your doctor about this if you consider opioids for your fibro.
One exception is a weak opioid called tramadol. Tramadol is an option for people with fibromyalgia if the usual medications don’t control symptoms. Besides its effect as a painkiller, tramadol affects neurotransmitter levels, which may partially work for fibro pain.
Tramadol shares side effects with opioids, so it can be habit-forming and tends to cause drowsiness. All opioids, including tramadol, should be avoided when driving or operating heavy machinery. If you have a history of seizures, you should avoid tramadol as it can lower your seizure threshold, meaning it can make it easier for a seizure to come on. Tramadol is the only opioid that has some known benefit in treating fibromyalgia.
What if my treatment is not working?
If your prescribed treatment is not working, your doctor will need to adjust your regimen. Treatment adjustment may include combining different medications or combining medication and a non-medication treatment. Be sure and let your doctor know if your treatment isn’t working. You can use the list of treatment options in this article for ideas to discuss further with your doctor.
Your doctor also might consider sending you to a specialist. Depending on what gives you the most trouble with your fibromyalgia, your doctor may refer you to a rheumatologist, physiatrist, physical therapist, psychologist/psychiatrist, sleep specialist, or pain management specialist.
Fibro and Other Chronic Pain Conditions
Many people with fibro have other painful conditions like migraine, arthritis, and irritable bowel syndrome. Treating these other pain sources can also help your fibro. With fibromyalgia, pain signals start in your brain and travel to target organs, such as your shoulders. In other conditions like arthritis, the pain signal starts in the target organ and gets transmitted to your brain. It is difficult for your doctor to determine where your pain signal originates if, for instance, you are feeling shoulder pain.
In the example of shoulder pain in someone with both arthritis and fibro, treating your arthritis would be the easiest first step in addressing your pain. Treatment may include medicines or trigger point injections. Trigger point injections involve injections into trigger points or areas of muscle spasm to decrease the pain and pain signals.
Complementary or alternative treatments might also be worth considering. You can refer yourself, or your doctor can refer you for alternative treatments. Your health insurance may require a physician referral for payment on alternative treatment programs. Be sure your doctor stays informed on all your therapies, even those you try on your own.
What are some alternative treatments for fibromyalgia?
The treatments with the best data in this category are yoga and tai chi. Both are safe for most people and can benefit many conditions besides fibro.
Yoga was started in ancient India and usually includes breathing exercises, simple meditation, and physical poses. There are many types of yoga. Some are more spiritual, while others build physical strength and flexibility. Yoga can increase your flexibility, strength, and muscle tone while allowing you to relax and decrease your stress and anxiety.
Tai chi originated in China and has its roots in self-defense as a martial art. Tai chi is a very graceful movement, and variations can include low-impact or more vigorous types. It also has a meditative component and can be helpful for stress reduction. Tai chi improves flexibility and strength, including your core muscle strength. Unlike yoga which focuses on posture, tai chi focuses on gentle, flowing movements.
Treatments that are less beneficial for fibromyalgia include acupuncture, Vitamin D, and transcranial magnetic stimulation.
The evidence is unclear with acupuncture on whether it helps fibro or not. Part of this may be because it is difficult to have very scientific studies about acupuncture as it is difficult to test against a placebo. You can discuss with your doctor whether you should try this.
- Vitamin D is most helpful for people who have a low Vitamin D level. Ask your doctor if you should have that level checked. Do not take high doses of Vitamin D (over 1000 units a day) without talking to your doctor, as Vitamin D does accumulate in your body and can have side effects if you get too much.
- Transcranial magnetic stimulation (TMS) is still in the initial stages of testing but has yielded promising results. TMS is a treatment where a magnet electrically stimulates the brain. Similar treatments are FDA (Food and Drug Administration) approved for depression and migraine.
- Low dose naltrexone. Naltrexone is a medication that blocks the effect of opioids in your body. Naltrexone is a medicine that treats alcoholism. Very low doses of naltrexone have been studied and found to be helpful in some conditions with central sensitization of pain, like fibromyalgia. However, just like TMS, studies are still in the early stages. TMS and low-dose naltrexone may be treatments doctors offer in the future.
Glossary
- Autoimmune disorders. Conditions where your body’s immune system, for unknown reasons, attacks a healthy part of your body, causing a disorder. For example, rheumatoid arthritis is an autoimmune disorder where your body’s immune system attacks your joints, causing arthritis.
- C-reactive protein (CRP)- A blood test that looks for inflammation in your blood.
- Central nervous system (CNS)- the nerves of your brain and spine.
- Central sensitization- a condition where your brain and spine are hypersensitive to pain signals. Central sensitization is involved in some chronic pain disorders.
- Chronic-something that lasts a long time, or something that never goes away.
- Clinical diagnosis-This is when your doctor determines what is wrong with you based on your symptoms and physical exam, not a blood test or x-ray.
- Cognitive Behavioral Therapy (CBT)-a type of psychotherapy, or counseling, that aims to change unhelpful thinking or behavioral patterns to help with various psychological problems.
- Diabetic neuropathy-nerve damage from diabetes. Diabetic neuropathy causes pain, numbness, tingling, and even weakness in your feet, hands, or even legs and arms when severe.
- Erythrocyte sedimentation rate (ESR)– a blood test that looks for inflammation in your blood.
- Gastrointestinal- relating to the stomach or intestines.
- Grey matter- the darker, outer layer of your brain. Grey matter helps in processing of information.
- Inflammatory markers- blood tests done to look for signs of inflammation in your body.
- Irritable bowel syndrome. (IBS)- an intestinal condition causing intermittent abdominal pain, bloating, diarrhea, gas, and constipation. The cause is unknown.
- Lyme disease-a disease caused by a bacteria called Borrelia that can cause a rash, arthritis, and other problems.
- Meditation- a type of training to focus your attention and rest your mind.
- Mindfulness- mentally focusing on what you are sensing and feeling now. Releasing thoughts of the past and the future. A type of meditation used to relax the body and mind and reduce stress.
- Myofascial pain syndrome- a chronic muscular pain disorder. A localized area of muscle pain and tenderness, often caused by repetitive overuse.
- Myositis. Inflammation of your muscles.
- Neurotransmitters- chemicals that nerves use to communicate with each other, as well as to communicate to other parts of the body.
- Obstructive sleep apnea (OSA)- condition where you intermittently stop breathing while you are sleeping.
- Opioids-also called narcotics. Many of these are medications used for pain control. These are all prone to habit-forming (addictive) and include morphine, oxycodone, hydromorphone, hydrocodone, fentanyl, and codeine. Street drugs that are opioids include heroin.
- Peripheral- in medicine, this is the opposite of central. When referring to your nerves, this refers to all your nerves outside of your brain and spine. This includes all the nerves that go to your arms, legs, internal organs, and skin.
- Peripheral Neuropathy-a disorder of the nerves of the legs and arms, often leading to chronic pain or numbness.
- Placebo-a placebo is a substance given to you that is not expected to be of any benefit. In a scientific study, placebos are pills made up of only sugar. They do not contain any medicine. Placebos (sugar pills) are given to half of the study participants; the other half receive the medication being studied. This allows the study to show the full benefits or side effects of the drug being studied.
- Polymyalgia rheumatica (PMR)- an uncommon and painful disorder in persons over 50yo involving inflammation in many muscles and joints.
- Post-traumatic stress disorder (PTSD)- mentally re-living a traumatic event for months or years. PTSD involves flashbacks, intrusive memories of the event, nightmares, anxiety, and depression.
- Progressive-something that gets worse over time.
- Raynaud’s syndrome- a condition where your fingers are affected by cold. The blood vessels become narrowed due to spasm. As a result, your fingers will temporarily change color and be numb and painful.
- Restless legs syndrome (RLS)- this is a disorder of your nerves that causes an extreme urge to move your legs, mostly at night.
- Rheumatoid arthritis-a type of autoimmune arthritis.
- Rheumatologist- a medical doctor who specializes in the diagnosis and treatment of arthritis, and other disorders of the whole body that affect the muscles and bones.
- Sedentary- state of inactivity. Spending most of your time sitting, doing little to no physical activity or exercise.
- Serotonin and norepinephrine reuptake inhibitors (SNRIs)- a class of medications used to treat depression, anxiety and some types of chronic pain. The name refers to the fact that the drugs affect the levels of serotonin and norepinephrine, neurotransmitters that your nerves use to communicate with each other, as part of how they work.
- Soft tissues-softer parts of your body, primarily fat or muscles under the skin.
- Stigma- when people have a negative attitude towards you because of a medical illness.
- Systemic Lupus Erythematosus (SLE), aka “Lupus”- An autoimmune disorder that affects multiple body parts including the skin, kidneys, joints, and brain.
- Physiatry-The medical specialty of Physical Medicine and Rehabilitation (PM & R). This type of doctor is a medical doctor, not a surgeon, who specializes in the rehabilitation of bone, muscle, and nerve disorders.
- Placebo-controlled Study– In this type of scientific research, half of the people in the study are given a medication or treatment, and the other half are given a placebo or “sugar pill.” None of the patients nor scientists know who has received the placebo and who the active treatment, until the end of the study. This type of study is more reliable than one that does not have a placebo control group.
- Raynaud’s phenomenon- a condition where the blood vessels in your fingers constrict in the cold, leading to your fingers becoming numb, cold, and pale.
- Referred pain- a pain that is felt outside of the area causing the pain. For example, pain in your arm when you have a heart attack is a type of referred pain.
- Tai Chi- a Chinese physical exercise to improve mindful movement.
- Tender point- areas in the soft tissue that are abnormally sensitive or tender to touch or pressure.
- Transcranial magnetic stimulation (TMS)-treatment where the brain is electrically stimulated by a magnet.
- Tricyclic antidepressants- a class of medications used to treat depression and some chronic pain conditions. The term “tricyclic” refers to the fact that these medications have three rings in their chemical structure.
- Trigger point- this is a specific spot in a tight band of muscle that when pressed is very irritable. Pressing on a trigger point will cause referred pain and may make the muscle visibly twitch.
- Trigger point injection- a small injection of a numbing medication, like lidocaine, into a tender muscle area. This is done in a doctor’s office.
- Yoga- ancient practice from India that involves postural poses.
Copyright: myObMD Media, LLC | Written by: Dayna Smith MD | Edited by: Lisa Shephard, MD | September 29, 2021
References
References
- Centers for Disease Control and Prevention , National Center for Chronic Disease Prevention and Health Promotion , Division of Population Health. https://www.cdc.gov/arthritis/basics/fibromyalgia.htm. Reviewed January 6, 2021. Accessed January 20, 2021.
- Goldenberg D. Clinical manifestations and diagnosis of fibromyalgia in adults. In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. Updated August 26, 2020. Accessed on January 20, 2021.
- Goldenberg D. Pathogenesis of fibromyalgia in. In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. Updated September 26, 2019. Accessed on January 20, 2021.
- Goldenberg D. Differential diagnosis of fibromyalgia in. In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. Updated July 9, 2020. Accessed on April 5, 2021.
- Goldenberg D. Initial treatment of fibromyalgia in adults. In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. Updated January 23,2020. Accessed on June 29, 2021.
- Goldenberg D. Treatment of fibromyalgia in adults not responsive to initial therapies. In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. Updated January 14,2020. Accessed on July 7, 2021.
- Top 10 Things to Know About the Second Edition of the Physical Activity Guidelines for Americans. US Department of Health and Human Services, Office of Disease Prevention and Health Promotion. https://health.gov/our-work/physical-activity/current-guidelines/top-10-things-know. Last updated October 7, 2020. Accessed July 10, 2021.
- Maness DL, Khan M. Nonpharmacologic Management of Chronic Insomnia. Am Fam Physician. 2015 Dec 15;92(12):1058-64. PMID: 26760592.
- Fibromyalgia: In Depth. US Department of Health and Human Services, National Institutes of Health, National Center for Complementary and Integrative Health. https://www.nccih.nih.gov/health/fibromyalgia-in-depth. Updated May 2016. Accessed July 10, 2021.
- Metyas S, Chen CL, Yeter K, Solyman J, Arkfeld DG. Low Dose Naltrexone in the Treatment of Fibromyalgia. Curr Rheumatol Rev. 2018;14(2):177-180. doi: 10.2174/1573397113666170321120329. PMID: 28325149.


